Dr Thivi Maruthappu and Professor Christopher Griffiths discuss the expanding role of nutrition in the management of common chronic skin conditions.
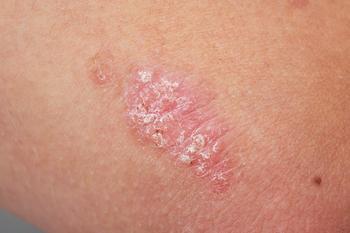
Psoriasis is a common chronic inflammatory skin condition that can have an enormous impact on quality of life. Affected individuals develop red, itchy and painful plaques on their skin with overlying scales that can cause both discomfort and shame. Medical management of psoriasis includes topical treatments such as vitamin D and steroid-based creams and ointments, light therapy and immunosuppressive medications such as methotrexate and ciclosporin. Over the last two decades, numerous biologic therapies have also been developed to treat psoriasis.
In recent years it has become apparent that the inflammation of psoriasis is not limited to the skin, but is also associated with the metabolic syndrome (including hypertension, non alcoholic fatty liver disease [NAFLD], insulin resistance, hyperlipidaemia and atherosclerosis). Epidemiological studies have strongly linked psoriasis to cardiovascular disease3 and obesity is a shared characteristic of this cluster of risk factors. Longitudinal population-based studies attribute a causal role for obesity in the development of psoriasis and psoriatic arthritis (PsA) linking it to increased disease severity and a 50% reduction in treatment response.4,5 Furthermore, a meta-analysis has demonstrated that a reduction in body mass index (BMI) of at least 5% in people with obesity and psoriasis resulted in a significant improvement in psoriasis severity.6
Despite this, there is a critical lack of evidence on the relationship between psoriasis and diet, nor is there specific, evidence-based guidance on diet for patients with psoriasis. Rather, recommendations are based on existing guidance for patients with cardiovascular disease. The Medical Board of the National Psoriasis Foundation in the USA strongly recommends dietary weight reduction with a hypocaloric diet in overweight and obese patients with psoriasis but fails to make specific dietary recommendations about which particular diet may be of benefit.7
The Mediterranean diet is one of the most highly studied dietary patterns, and has consistently demonstrated utility in reducing the incidence of major cardiovascular events in high-risk individuals when compared with a low-fat diet.8 The traditional Mediterranean diet is characterised by a high intake of olive oil, fruit, nuts, vegetables and cereals, a moderate intake of fish and poultry and a low intake of dairy, red meat, processed meats and refined sugars.9 Observational studies have identified low levels of adherence to a Mediterranean diet in patients with severe psoriasis; olive oil and fish consumption are independently predictive for PASI (Psoriasis Activity and Severity Index) and C-reactive protein levels.10,11 The authors of these studies attribute the Mediterranean diet’s ability to reduce chronic systemic inflammation to the anti-inflammatory properties of dietary fibres, antioxidants and polyphenols that are rich in this pattern of eating.
Recently there has been growing interest in the role of temporal patterns of energy intake across the day and intermittent energy restriction in the management of a number of chronic inflammatory states such as the metabolic syndrome, arthritis and multiple sclerosis. However, to date, no studies have explored whether restriction of eating time windows could be effective in the management of psoriasis.
The APPLE study will explore this in two ways – firstly a cross-sectional observational study of patients with psoriasis to examine current dietary patterns and compare these with the UK control population. The second aspect of the study will conduct a small clinical trial comparing a Mediterranean-style diet with a time-restricted Mediterranean style diet, assessing several clinical and biochemical parameters to determine response. We hope that this study will help to shed light on the role of nutrition in the management of psoriasis.
Knowledge booster
- Psoriasis is a chronic inflammatory skin disease that affects 2-4% of the UK population with a rising prevalence and a substantial impact on quality of life.1
- It is characterised by the presence of painful and itchy red scaly patches on the skin.2
- There is a growing body of evidence to support the role of dietary interventions in the management of psoriasis.
- Psoriasis is linked to cardiovascular disease and consequent increased morbidity and mortality.
- Nutrition and dietetics guidance is a priority for patients with psoriasis however, such resources are at present limited.
- The role of diet and nutrition in the management of psoriasis is a frequent question asked by people living with this chronic, currently incurable skin disease.
- At present, limited evidence-based guidance on diet and nutrition exists for psoriasis patients and their families.
- Studies have shown that weight loss in people with psoriasis who are overweight or obese can result in significant improvements in the severity of their skin condition.
- Psoriasis has been independently linked to ischaemic heart disease, Type 2 diabetes, hyperlipidaemia and hypertension
- The APPLE Study (Asking People with Psoriasis about Lifestyle and Eating) is the first study of its kind in the UK bringing together Dermatologists and researchers in Nutrition Science) to help address one of the commonest questions that patients with psoriasis pose “will changing what I eat help my skin condition?”
- As there is a lack of evidence-based guidance, people with psoriasis invariably explore dietary exclusions such as “gluten-free” or “dairy free” diets in an attempt to improve their skin, typically with limited success.
References
- Icen M, Crowson CS, McEvoy MT et al. Trends in incidence of adultonset psoriasis over three decades: a population-based study.
- Griffiths CEM, Armstrong AW, Gudjonsson JE, Barker JNWN. Psoriasis. Lancet. 2021 Apr 3;397(10281):1301-1315
- Takeshita J, Grewal S, Langan SM et al. Psoriasis and comorbid diseases: epidemiology. J Am Acad Dermatol 2017; 76:377–90
- Armstrong AW, Harskamp CT, Armstrong EJ. The association between psoriasis and obesity: a systematic review and meta-analysis of observational studies. Nutr Diabetes 2012; 2:e54
- Hojgaard P, Glintborg B, Kristensen LE et al. The in uence of obesity on response to tumour necrosis factor-a inhibitors in psoriatic arthritis: results from the DANBIO and ICEBIO registries. Rheumatology (Oxford) 2016; 55:2191–9
- Mahil, S., McSweeney, S., Kloczko, E., McGowan, B., Barker, J. and Smith, C. (2019), Does weight loss reduce the severity and incidence of psoriasis or psoriatic arthritis? A Critically Appraised Topic. Br J Dermatol, 181: 946-953
- Ford AR, Siegel M, Bagel J, et al. Dietary Recommendations for Adults With Psoriasis or Psoriatic Arthritis From the Medical Board of the National Psoriasis Foundation: A Systematic Review. JAMA Dermatol. 2018;154(8):934–950
- Papadaki A, Nolen-Doerr E, Mantzoros CS. The Effect of the Mediterranean Diet on Metabolic Health: A Systematic Review and Meta-Analysis of Controlled Trials in Adults. Nutrients. 2020 Oct 30;12(11):E3342
- Estruch R, Ros E, Salas-Salvad J, Covas MI, Corella D, Ar s F, G mez-Gracia E, Ruiz-Guti rrez V, Fiol M, Lapetra J, Lamuela-Raventos RM, Serra-Majem L, Pint X, Basora J, Mu oz MA, Sorl JV, Mart nez JA, Mart nez-Gonz lez MA. Retraction and Republication: Primary Prevention of Cardiovascular Disease with a Mediterranean Diet. N Engl J Med 2013;368:1279-90. N Engl J Med. 2018 Jun 21;378(25):2441-2442
- Korovesi A, Dalamaga M, Kotopouli M, Papadavid E. Adherence to the Mediterranean diet is independently associated with psoriasis risk, severity, and quality of life: a cross-sectional observational study. Int J Dermatol. 2019 Sep;58(9):e164-e165
- Phan C, Touvier M, Kesse-Guyot E, Adjibade M, Hercberg S, Wolkenstein P, Chosidow O, Ezzedine K, Sbidian E. Association Between Mediterranean Antiinflammatory Dietary Profile and Severity of Psoriasis: Results From the NutriNet-Sant Cohort. JAMA Dermatol. 2018 Sep 1;154(9):1017-1024

