There are many different 'tests' available to diagnose food allergy or food intolerance. It can be difficult to know which are reliable or based on science. This fact sheet will examine the tests available and whether they are based on evidence.
What is the difference between food allergy and food intolerance?
Eating certain foods may lead to an unpleasant - and sometimes dangerous - physical reaction in some people.
A 'food allergy' is a reaction that involves the immune system, which is the body’s defence against foreign bodies. Those that do not involve the immune system are often called a ‘food intolerance’. Find out more in our food allergy and intolerance fact sheet.
Common food allergy terms
Medical terms for food allergy and intolerance can be confusing. Here are some common terms and what they mean.
Food hypersensitivity
Covers all abnormal reactions to food.
IgE mediated food allergy
This reaction involves IgE antibodies, which your immune system produces. The signs and symptoms of the reaction are rapid and can be severe. Conventional allergy testing, and a detailed allergy-focused clinical history, can help with diagnosis.
Non-IgE mediated food allergy
This reaction involves the immune system, but not IgE antibodies. Signs and symptoms of a reaction are delayed or ‘slow onset’. Allergy testing is not helpful. Exclusion and reintroduction of the suspected 'culprit' food(s) lead to diagnosis.
Non-allergic food hypersensitivity
The immune system is not involved in this type of reaction. It is also known as food intolerance. Exclusion and reintroduction of the suspected 'culprit' food(s) lead to diagnosis.
Conventional Allergy Testing
These tests are evidence-based and performed by registered health professionals.
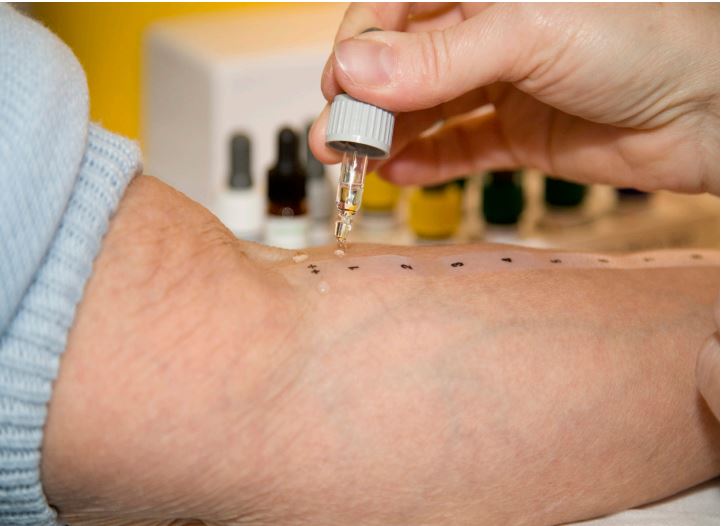
Skin prick test
A small amount of diluted allergen (the protein we suspect you are allergic to) is placed on your skin and then your skin is pricked. If a small swollen lump or ‘weal’ appears, in conjunction with a detailed clinical history, an IgE mediated food allergy may be diagnosed. This test is only performed under medical supervision.
Blood tests
A specific IgE test measures the amount of IgE antibodies to a suspect food in the blood. This is called a Radio Allergo Sorbent Test (RAST). Your results will give a diagnosis of IgE mediated food allergy (along with a detailed clinical history). Your GP or hospital clinician can organise this blood test.
Commercial companies may offer a similar blood test called MAST (Multi-Allergen Screening Test). However, it is difficult to give an accurate diagnosis without your full clinical history.
Food challenges
Starting with a small amount, you will be given the suspect food orally (in the mouth). Your clinician will gradually increase the amount, checking to see if you have any symptoms. You may be aware of the food you are eating, or 'blinded' and unaware of which food you are eating. This test should only be performed under medical supervision with medical facilities and resuscitation equipment available.
Food exclusion and reintroduction
You stop eating the suspected food(s) for a period of time and watch and record your symptoms. If your symptoms improve, then the suspect food is reintroduced. If your symptoms return, this would indicate a problem with that particular food.
This test can be very time consuming. It is best carried out under the supervision of a registered dietitian, especially if involving children. A well-balanced nutritional intake during the test period is important - especially if you are excluding major food groups like dairy or wheat.
Alternative tests
There are also many commercially available tests that claim to diagnose food hypersensitivity.
You should avoid these because they have no scientific basis. They can be harmful when multiple foods are excluded without reason, or if they are not reintroduced under guidance of a dietitian.
IgG blood test
This blood test looks at IgG antibodies to specific foods present in your blood. The test claims that an increase in IgG to a certain food indicates intolerance to that food. IgG antibodies to food are found in all healthy adults & children who do not show any symptoms.
There is currently no convincing evidence to support this test and it is not recommended as a diagnostic tool.
Kinesiology
This is based on the idea that certain foods cause an energy imbalance in the body which is detected by testing the response of the muscle. The therapist would test your muscle response when holding the suspect food in a glass vial.
Studies show that this test is no better than chance and is not recommended.
Hair analysis
A small lock of your hair is sent to a laboratory, where they scan the energy fields in the hair. The results are then compared to a database.
This testing is used for recreational drug use and lead and mercury poisoning. However, its use in allergy testing is unproven and has no scientific basis.
The ATCAT (Antigen Leucocyte cellular antibody Test)
Your white blood cells are mixed with the suspect food. It is claimed that changes in the size of the white blood cells indicate a problem with that food.
There is no rational scientific basis for this test.
Pulse test
Your pulse is taken before eating the suspect food and then 15 minutes afterwards. It is claimed that an increase of ten beats per minute indicates food intolerance.
Research shows there is no connection between an increased pulse and food intolerance.
Electrodermal (Vega) test
This test measures the electromagnetic conductivity in your body. It is claimed that an offending food will show a dip in the electromagnetic conductivity.
Research studies show that this test is no better than chance.
Provocation – Neutralization testing
Food extracts are injected under your skin to try and cause food related symptoms previously reported. A different dose of the food extract is then injected to ‘neutralise’ the reaction.
There is no rational scientific basis for this test.
The problem with non-evidenced tests
These alternative allergy tests are not based in scientific evidence. They are a waste of your money and may suggest long lists of foods to be excluded from the diet unnecessarily.
Excluding a major food group e.g. wheat or milk, or a combination of different foods, can cause many difficulties. Without proper nutritional advice, a restricted diet can lead to nutritional deficiencies, malnutrition and reduced quality of life.
Summary
- If you think you may have a food allergy, seek proper medical advice. They will discuss the use of evidence-based, conventional allergy testing.
- Alternative allergy testing should be avoided as it has no scientific basis.
- Dietitians can give you the correct nutritional advice and ensure a well-balanced nutritional intake that will be tasty, varied and culturally acceptable.
- Children should not follow a restricted diet unless supervised by a paediatric dietitian as they need a well-balanced diet to ensure adequate growth and development.
Source(s)
Atkinson W., Sheldon T.A., Shaath N., Whorwell P.J. (2004) Food elimination based on IgG antibodies in irritable bowel syndrome: a randomised controlled trial. Gut 53: 1459-1464
The British Society for Allergy & Clinical Immunology (BSACI) [accessed 16 February 2021]. Available from: https://www.bsaci.org/
Ernst E. (2000) The role of complementary and alternative medicine. BMJ 321: 1133-1135
Engler RJ, Gregory, PJ. and Jellin, JM. (2009) Complementary and alternative medicine for the allergist immunologist: Where do I start? J Allergy Clin Immunol 123(2):309-16
NICE (2011) Guidelines on Diagnosis and Assessment of Food Allergy in Children and Young People in Primary Care and Community Setting NICE Clinical Guideline no 116
Ives A.J. and Hourihane J. O'B. (2002) Evidence-based diagnosis of food allergy. Current Paediatrics 12: 357-364
Kelso, J.M (2018). Unproven Diagnostic Tests for adverse Reactions to Foods. J Allergy Clin Immunol, Pract;6:362-365
Niggemann B. and Gruber C. (2003) Side-effects of complementary and alternative medicine. Allergy 58: 707-716
Niggemann B. and Gruber C. (2004) Unproven diagnostic procedures in IgE-mediated allergic diseases. Allergy 59(8): 806-808
Pothmann R et al (2001) Evaluation of applied kinesiology in nutritional intolerance of childhood. Research in complementary and natural classical medicine 8(6): 336 44
Stapel, S.O., Asero, R., Ballmer-Weber, B.L., Know, E.F., Strobel, S. et al. (2008) Testing for IgG4 against foods is not recommended as a diagnostic tool. EAACI Task Force Report Allergy 63 793-6
Teuber S.S and Porch-Curren C (2003) Unproved diagnostic and therapeutic approaches to food allergy and intolerance. Current Opinion in Allergy and Clinical Immunology 3(3): 217-221
Wisniewski, J.A. and Li, X (2012) Alternative and Complementary Treatment for Food Allergy Immunology and Allergy Clinics of North America, Volume 32, Issue 1, Pages 135-150







